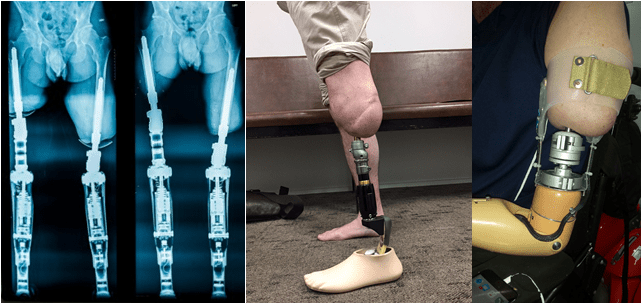
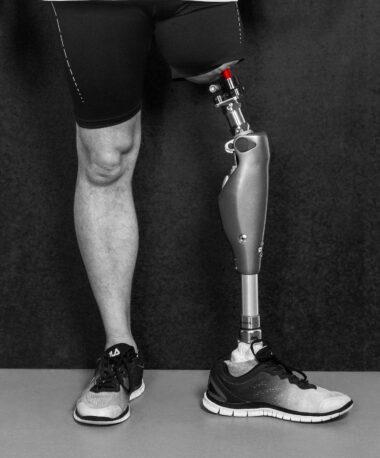
People with above or below knee amputations seek to return to a mobile lifestyle. Conventional rehabilitation uses a socket prosthesis, which is fixed to the soft tissue of the remaining amputation stump via suction or vacuum. The artificial knee joint and/ or lower leg prosthesis can then be attached to the socket. This enables the patients to walk without aids but there are several challenges in the use of a suction prosthesis. One important factor is the length of the remaining stump because it determines the lever arm and the force, which has to be applied for conducting, guiding, and controlling the prosthesis. If the socket does not fit properly it can create skin irritations of the soft tissue, which may lead to sores, ulcers, chronic inflammation with abscesses, and pain.
Moreover, the remaining stump length correlates with the energy expenditure during walking and an amputee uses on average 70% more energy than an able-bodied person. These difficulties can result in a poor gait with negative effects on the remaining musculoskeletal system. This often leads amputees to utilize walking aids or even a wheelchair.
Hence a prosthesis that avoids the skin and soft tissue interface is desirable for different reasons:
– Skin irritation due to friction, chaffing, and squeezing
– An increase in sweating and heat rashes
– Inflammation, bruises and hematoma, pressure marks, and even deep skin injuries
– The dissatisfying fit of the prosthesis due to variation of weight and stump volume
– Pain and missing comfort also during sitting
– Hygienic problems
For a lot of amputees, it is therefore difficult to find their way back into an active lifestyle or to the working force. Often they cannot perform the kind of activity and sports, which they would like to enjoy and they have to rely on the help of others during everyday life. Because of the mentioned difficulties, some single-side or bilateral amputees even depend on a wheelchair permanently.
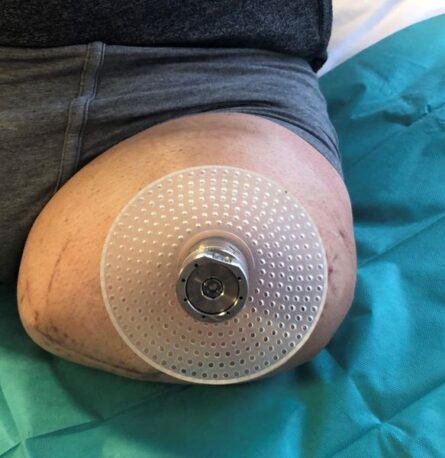
An osseointegrated, transcutaneous implant creates an alternative to these problems. “Osseointegrated” means “fixed to the bone” and transcutaneous is “perforating the skin”. With this system, the prosthesis is directly attached to the bone and a socket or suction prosthesis becomes unnecessary and dispensable.
 English
English
 English
English
 English
English